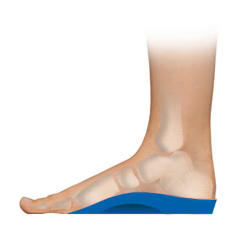
Plantar Fasciitis (heel pain)
Footlogic: The science of walking comfort
Articles in this section
Symptoms:

Consistent with plantar fasciitis are shortened/tight gastrocnemius muscles. This can be evidenced by the inability to perform the “flying frog” position. In flying frog the patient goes into a full squat position and maintains balance and full ground contact with the sole of the foot. Elevation of the heel signifies a tight gastroc complex.
Causes:

By far the most common cause of plantar fasciitis is faulty biomechanics of the lower limb. Excessive subtalar joint pronation lowers the arch structure causing the foot to elongate abnormally, placing excess traction forces on the plantar fascia. Prolonged tractional forces will result in inflammation and micro-tearing of the fascia and surrounding tissues, causing pain in the heel (and sometimes in the arch area). In some cases a bony growth will develop on the calcaneal tuberosity, referred to as a heel spur.
Tight calf muscles can add to plantar fascial stress. A tight gastroc holds the foot in a pronated position, decreasing the foot’s ability to supinate on ground contact and toe-off. In other words, the foot cannot dorsiflex at the level of the ankle during the propulsive phase of gait, resulting in the foot dorsiflexing at the midtarsal joint which then places strain on the plantar fascia.
Excessively high arches may also predispose the foot to plantar fasciitis. The high arch-plantar fasciitis theory points to the windlass mechanism. During the toe-off phase the toes are dorsiflexed. The arch rises up into a packed position making the foot a rigid lever and the plantar fascia is tractioned tight by the dorsiflexed toes. The higher the arch the greater the potential range of motion. The increased stresses on the foot from biomechanical deficiency may produce micro-tears that develop into plantar fasciitis.
A frequently overlooked cause is the role myofascial trigger points play in disrupting the joint mechanics of the foot. Trigger points in the muscles of the leg (gastroc, soleus, peronei, anterior tibialis) can disrupt proper biomechanics of the foot and ankle through the phases of ground contact, disrupting the supination-pronation-supination sequence. Trigger points are due to direct muscular fatigue, direct trauma or chilling. The gastroc and soleus muscles play an important role in body posture and are therefore under stress throughout upright movements. Lumpy areas, areas of point tenderness or a hard feel may indicate trigger points.
Treatment:
Orthotic therapy should be considered as a treatment option for plantar fasciitis. Footlogics orthotics will aid in the control of excessive pronation and will assist the arch in rising, thus greatly reducing plantar fascial traction forces. If the condition is treated in its early stages, orthotics will help prevent a calcaneal spur from developing.
Surgery (i.e. removal of heel spurs and/or surgical plantar fascial release) is seldom required and should only be considered as a last resort.
Importantly, the patient should stretch the calf muscles several times a day. Other useful exercises are: massaging the plantar fascia by rolling a ball or under the foot, stretching the plantar fascia by grabbing the toes and pulling them towards the shin (hold for about 15 seconds).
Additional treatment options include: rest/reduced activity, hot/cold therapy, anti-inflammatories, shockwave therapy and wearing a night splint.